|
11/13/2023 0 Comments Mog disease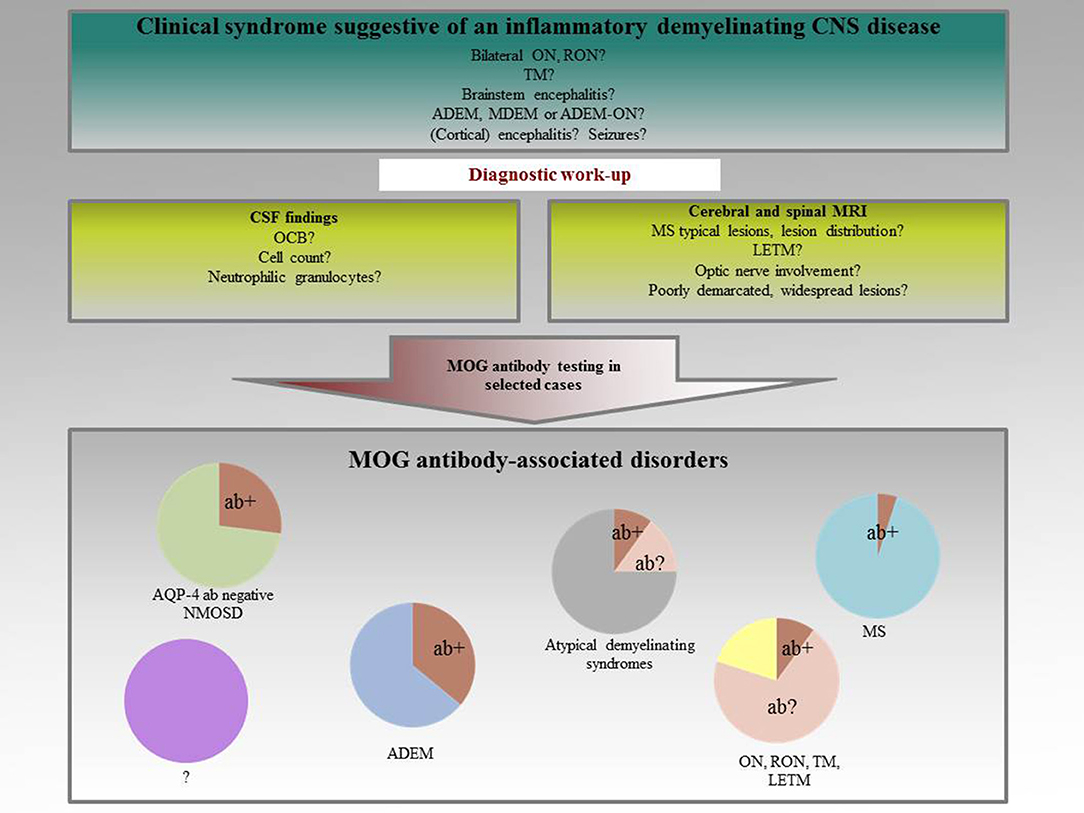
As the clinical spectrum of MOGAD continues to expand, so too does our appreciation for diagnostic and management challenges associated with this enigmatic condition. Occasionally, patients with MOGAD have an overlap syndrome with anti-NMDA receptor encephalitis, characterized by clinical features of demyelination associated with encephalopathy, seizures, dyskinesias, or psychosis. Yet, disease manifestations may occur after prodromal infections, particularly those caused by viral pathogens, such as influenza, Epstein–Barr virus, herpes simplex virus, and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), to name a few. Unlike NMOSD, cases of MOGAD are not strongly associated with other systemic autoimmune disorders or circulating autoantibodies. Notably, these numbers, along with the estimated worldwide prevalence of 20 million, are likely to increase with growing recognition of the disease and improved availability of serological testing. The current estimated range of incidence in the pediatric population is 3.1 per 1 million, as compared to 1.6 and 2.39 per 1 million among adults. MOGAD also has the greatest predilection in children, representing 20–30% of inflammatory CNS syndromes in this population as compared to approximately 5% in adults. While patients with MS, MOGAD and NMOSD may present with similar clinical manifestations, such as optic neuritis and myelitis, those with MOGAD lack a clear sex predilection, and more commonly experience a monophasic course. CNS inflammatory demyelinating conditions, including multiple sclerosis (MS) and neuromyelitis optica spectrum disorders (NMOSD), are differentiated based on severity, clinical phenotype, imaging, laboratory, and pathological findings (Table 1). Myelin oligodendrocyte glycoprotein antibody-associated disease (MOGAD) is a relatively new addition to the category of central nervous system (CNS) inflammatory demyelinating diseases. Key challenges to the current understanding of MOGAD are also highlighted, including uncertainty regarding the specificity and pathogenicity of MOG autoantibodies, the need to identify immunopathologic targets for future therapies, the quest to validate biomarkers that facilitate diagnosis and detect disease activity, and the importance of deciphering which patients with MOGAD require long-term immunotherapy. In this review, cardinal clinical features of MOGAD are discussed. For this reason, possible alternative diagnoses need to be considered, and low MOG-IgG titers need to be carefully weighted. Over the last several years, access to cell-based assay (CBA) techniques has improved diagnostic accuracy, yet the positive predictive value of serum MOG-IgG values varies with the prevalence of MOGAD in any given patient population. Seropositivity status for MOG-IgG autoantibodies is important for diagnosing MOGAD, but only in the context of robust clinical characterization and cautious interpretation of neuroimaging. New diagnostic criteria for myelin oligodendrocyte glycoprotein antibody-associated disease (MOGAD) have recently been proposed, distinguishing this syndrome from other inflammatory diseases of the central nervous system.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
